Tiny white bumps keep showing up on my eyelids, and I can’t get in to be seen yet. What are these?
 1. What Tiny White Bumps on the Eyelids Usually Are
The tiny white bumps on your eyelids are most commonly known as milia. Milia are small, keratin-filled cysts that form just under the surface of the skin. They are typically 1 to 2 millimeters in size and have a pearly-white appearance. Unlike acne, milia are not caused by clogged pores or bacterial infections.
Milia can occur at any age and are particularly common in newborns. However, they can also develop in adults, especially around the eye area where the skin is delicate and thin. They are usually harmless and not associated with any underlying medical condition.
2. Milia 101: Why These Little Cysts Form Around the Eyes
Milia form when dead skin cells become trapped in small pockets near the skin's surface instead of exfoliating naturally. This trapped keratin becomes a tiny cyst. The formation of milia is not fully understood, but it is believed to be related to skin damage, such as from sun exposure, or the use of heavy skincare products that can clog the skin's surface.
The eye area is particularly prone to milia because the skin is thinner and more sensitive to environmental damage and product buildup. People who use thick creams or heavy makeup around the eyes without proper cleansing may be more susceptible to developing milia.
3. How to Tell Milia From a Stye, Chalazion, or Whitehead
Distinguishing milia from other eyelid conditions is essential for proper management. Milia are firm, white, and painless bumps that do not change much in size. A stye, on the other hand, is a red, painful lump near the edge of the eyelid, caused by an infection of an oil gland. Styes are often tender to the touch and can cause swelling of the eyelid.
A chalazion is similar to a stye but is usually larger, less painful, and occurs further back on the eyelid. Chalazia result from a blocked oil gland and can take longer to resolve. Whiteheads, unlike milia, are soft, filled with pus, and often part of acne breakouts.
4. Red-Flag Symptoms That Mean You Should Seek Urgent Care
While milia are generally harmless, certain symptoms may indicate a more serious issue that requires immediate medical attention. If you experience severe pain, significant swelling, redness, or any vision changes, it's crucial to seek urgent care. These could be signs of an infection or other eye conditions that need prompt treatment.
Additionally, if the bumps are rapidly changing in size or appearance, or if there is any discharge, it's advisable to contact a healthcare professional as soon as possible to rule out other conditions.
5. Everyday Habits and Products That Can Trigger Milia
Certain habits and skincare products can contribute to the development of milia. Using heavy creams or oil-based products around the eyes, especially without thorough cleansing, can lead to clogged skin and milia formation. Sun damage is another factor, as it can lead to thicker skin and more dead skin cell buildup.
Exfoliating too aggressively or using harsh products can irritate the skin and contribute to milia. It's essential to maintain a balanced skincare routine that includes gentle cleansing and moisturizing while avoiding overly rich products.
6. Safe At-Home Steps While You’re Waiting for an Appointment
While waiting to see a healthcare professional, there are several safe steps you can take at home to manage milia. Start by keeping the eye area clean and free from heavy creams and makeup. Use a gentle cleanser to wash your face and avoid scrubbing the delicate skin around your eyes.
Applying a warm compress to the affected area can help soften the skin and may facilitate the natural exfoliation process. Consider using a mild exfoliating product containing ingredients like salicylic acid or glycolic acid, but be cautious to avoid irritation.
7. Treatments an Eye Doctor or Dermatologist Might Recommend
Once you see a healthcare professional, they may recommend various treatments depending on the severity of the milia. In some cases, they might suggest a topical retinoid cream to help exfoliate the skin and promote cell turnover.
For more persistent milia, a dermatologist may perform a procedure called de-roofing, where they use a sterile needle to remove the cyst. Laser treatments or microdermabrasion might also be options for more extensive cases.
8. What Not to Do: Squeezing, Popping, and DIY Surgery Risks
It's important to avoid squeezing or attempting to pop milia, as this can lead to skin damage, scarring, and potential infection. DIY removal attempts can cause more harm than good, especially in the delicate eye area.
Using unsterile tools or incorrect techniques can introduce bacteria and result in complications. It's always best to leave removal to a professional who can perform the procedure safely and effectively.
9. When Tiny White Bumps Aren’t Milia: Other Possible Causes
While milia are common, other conditions can also cause white bumps on the eyelids. Sebaceous cysts, xanthelasma (yellowish cholesterol deposits), or syringomas (sweat gland tumors) may appear similar to milia.
Each condition has distinct characteristics and may require different treatments. A healthcare professional can provide an accurate diagnosis and appropriate management plan for these conditions.
10. How to Help Prevent Milia From Coming Back
Preventing milia involves maintaining good skincare practices. Use non-comedogenic (non-pore-clogging) products and ensure thorough cleansing, especially around the eyes. Incorporate a gentle exfoliant into your routine to help remove dead skin cells.
Protecting your skin from sun exposure by wearing sunscreen and sunglasses can also reduce the risk of milia. Regular skin check-ups with a dermatologist can help address any concerns early and maintain healthy skin.
11. Questions to Ask Your Doctor Once You Finally Get Seen
When you finally have your appointment, consider asking your doctor specific questions to understand your condition better. Inquire about the exact diagnosis and whether the bumps are indeed milia. Ask about the recommended treatments and any potential side effects or downtime.
Discuss preventive measures to avoid recurrence and any lifestyle changes that might be beneficial. Understanding the nature of your condition and how to manage it can empower you to take charge of your skin health.
1. What Tiny White Bumps on the Eyelids Usually Are
The tiny white bumps on your eyelids are most commonly known as milia. Milia are small, keratin-filled cysts that form just under the surface of the skin. They are typically 1 to 2 millimeters in size and have a pearly-white appearance. Unlike acne, milia are not caused by clogged pores or bacterial infections.
Milia can occur at any age and are particularly common in newborns. However, they can also develop in adults, especially around the eye area where the skin is delicate and thin. They are usually harmless and not associated with any underlying medical condition.
2. Milia 101: Why These Little Cysts Form Around the Eyes
Milia form when dead skin cells become trapped in small pockets near the skin's surface instead of exfoliating naturally. This trapped keratin becomes a tiny cyst. The formation of milia is not fully understood, but it is believed to be related to skin damage, such as from sun exposure, or the use of heavy skincare products that can clog the skin's surface.
The eye area is particularly prone to milia because the skin is thinner and more sensitive to environmental damage and product buildup. People who use thick creams or heavy makeup around the eyes without proper cleansing may be more susceptible to developing milia.
3. How to Tell Milia From a Stye, Chalazion, or Whitehead
Distinguishing milia from other eyelid conditions is essential for proper management. Milia are firm, white, and painless bumps that do not change much in size. A stye, on the other hand, is a red, painful lump near the edge of the eyelid, caused by an infection of an oil gland. Styes are often tender to the touch and can cause swelling of the eyelid.
A chalazion is similar to a stye but is usually larger, less painful, and occurs further back on the eyelid. Chalazia result from a blocked oil gland and can take longer to resolve. Whiteheads, unlike milia, are soft, filled with pus, and often part of acne breakouts.
4. Red-Flag Symptoms That Mean You Should Seek Urgent Care
While milia are generally harmless, certain symptoms may indicate a more serious issue that requires immediate medical attention. If you experience severe pain, significant swelling, redness, or any vision changes, it's crucial to seek urgent care. These could be signs of an infection or other eye conditions that need prompt treatment.
Additionally, if the bumps are rapidly changing in size or appearance, or if there is any discharge, it's advisable to contact a healthcare professional as soon as possible to rule out other conditions.
5. Everyday Habits and Products That Can Trigger Milia
Certain habits and skincare products can contribute to the development of milia. Using heavy creams or oil-based products around the eyes, especially without thorough cleansing, can lead to clogged skin and milia formation. Sun damage is another factor, as it can lead to thicker skin and more dead skin cell buildup.
Exfoliating too aggressively or using harsh products can irritate the skin and contribute to milia. It's essential to maintain a balanced skincare routine that includes gentle cleansing and moisturizing while avoiding overly rich products.
6. Safe At-Home Steps While You’re Waiting for an Appointment
While waiting to see a healthcare professional, there are several safe steps you can take at home to manage milia. Start by keeping the eye area clean and free from heavy creams and makeup. Use a gentle cleanser to wash your face and avoid scrubbing the delicate skin around your eyes.
Applying a warm compress to the affected area can help soften the skin and may facilitate the natural exfoliation process. Consider using a mild exfoliating product containing ingredients like salicylic acid or glycolic acid, but be cautious to avoid irritation.
7. Treatments an Eye Doctor or Dermatologist Might Recommend
Once you see a healthcare professional, they may recommend various treatments depending on the severity of the milia. In some cases, they might suggest a topical retinoid cream to help exfoliate the skin and promote cell turnover.
For more persistent milia, a dermatologist may perform a procedure called de-roofing, where they use a sterile needle to remove the cyst. Laser treatments or microdermabrasion might also be options for more extensive cases.
8. What Not to Do: Squeezing, Popping, and DIY Surgery Risks
It's important to avoid squeezing or attempting to pop milia, as this can lead to skin damage, scarring, and potential infection. DIY removal attempts can cause more harm than good, especially in the delicate eye area.
Using unsterile tools or incorrect techniques can introduce bacteria and result in complications. It's always best to leave removal to a professional who can perform the procedure safely and effectively.
9. When Tiny White Bumps Aren’t Milia: Other Possible Causes
While milia are common, other conditions can also cause white bumps on the eyelids. Sebaceous cysts, xanthelasma (yellowish cholesterol deposits), or syringomas (sweat gland tumors) may appear similar to milia.
Each condition has distinct characteristics and may require different treatments. A healthcare professional can provide an accurate diagnosis and appropriate management plan for these conditions.
10. How to Help Prevent Milia From Coming Back
Preventing milia involves maintaining good skincare practices. Use non-comedogenic (non-pore-clogging) products and ensure thorough cleansing, especially around the eyes. Incorporate a gentle exfoliant into your routine to help remove dead skin cells.
Protecting your skin from sun exposure by wearing sunscreen and sunglasses can also reduce the risk of milia. Regular skin check-ups with a dermatologist can help address any concerns early and maintain healthy skin.
11. Questions to Ask Your Doctor Once You Finally Get Seen
When you finally have your appointment, consider asking your doctor specific questions to understand your condition better. Inquire about the exact diagnosis and whether the bumps are indeed milia. Ask about the recommended treatments and any potential side effects or downtime.
Discuss preventive measures to avoid recurrence and any lifestyle changes that might be beneficial. Understanding the nature of your condition and how to manage it can empower you to take charge of your skin health.
6 habits that make older women look beautiful
The idea of beauty is one of those rare things in life that becomes more intriguing as time goes by. When we are young, beauty is a purely biological thing, something that happens because of our genetic makeup and our youthful, smooth skin. But as we age, so does our understanding of beauty. Not only does beauty not disappear; it changes, becoming more complex and profound. It evolves from an aesthetic aspect into a deeper notion.
Many women become elegant in a certain way. They develop an aura of quiet confidence, poise, and charisma that is unique to them and impossible to buy or copy. Their beauty doesn’t come as a result of trendy, costly procedures and treatments, but is the product of habits cultivated over many years.
Instead of seeking perfection, which is an impossible and ultimately tiresome goal by its very definition, it’s more realistic to focus on growth and self-respect.
The following is an analysis of several traits that make up a woman’s natural beauty as she matures, as well as the rationale behind why they work for her mind and body.

The Art of Posture and Intentional Movement
A person’s posture can say more before any hello than their actual words. Body language is perhaps the most primitive means of communication and conveys what the mind truly feels. Standing straight, keeping one’s shoulders relaxed instead of hunched up by the ears, and moving with purpose convey an impression of self-confidence.
Of course, as people age, some deterioration of posture occurs. This can be attributed to the weakening of muscles, decreased bone density, and the effects of years of poor posture, which often develop from sitting too long at a desk or staring at smartphones. However, recent discoveries in the science of “embodied cognition” have shown that posture does not only affect other people’s perception but also influences one’s inner state. When a person stands tall, they do not only “pretend” to be confident—they signal to their brain that they are comfortable and in control of their surroundings.
Women who pay attention to maintaining good posture look more lively and youthful, since they do not seem to “age down” into themselves. A smooth, stable walking pattern, together with an upright posture, helps create a sense of elegance that has nothing to do with what brand name one wears or how professionally one’s make-up is applied.

Radical Consistency in Self-Care
Good skin is not about an elaborate and lengthy nighttime regimen of cutting-edge ingredients. Instead, dermatological studies continually emphasize one simple yet critical truth: consistency wins over complexity. Women who radiate health despite their advanced age are often those who have stopped playing around with each new trend and developed a trustworthy and basic routine.
Skincare for graceful aging can be simplified to the three core steps: cleansing, moisturizing, and protection. In particular, the latter step is proven to be crucial to prevent premature aging of the skin. It is believed that 80% to 90% of visible signs of skin aging, such as wrinkles, dryness, and uneven skin tone, are due to excessive exposure to the sun. For instance, women who apply a daily layer of SPF for twenty years differ noticeably from those who only do so when going to the beach.
The next pillar is moisturization. As you get older, your skin barrier weakens, becoming less effective at retaining lipids and moisture. By hydrating the skin, you support this barrier, which keeps the skin soft, glowing, and more resistant to damage from external factors. It’s not about how expensive the jar is, it’s about consistency. These women care for their skin as an investment, not as an emergency that requires miracle fixes.
Personal Style Over Fleeting Trends
There is a vast difference between being “fashionable” and “having style.” The former dictates what one should wear according to fashion industry standards each month, while the latter is choosing to wear clothes that define one’s identity. In the development of one’s sense of beauty, many ladies experience a significant boost in confidence once they cease trying to fit in with fashion standards tailored to adolescents and begin building an individual aesthetic reflective of who they are now.
It is important to note that this is not about one’s selfish interests but rather a phenomenon known as “enclothed cognition.” The hypothesis posits that the clothing one wears can actually affect their psychology. When women dress themselves up in clothes that suit their body type, make them feel comfortable, and reflect their character.
As women age and become unique in their looks, they usually go for clothing that complements their body and accentuates their facial features rather than concealing their true beauty by wearing clothes that are too big for them or too small. Women who have unique looks usually become experts at color matching. They know what colors bring out the best in them and which colors are just not flattering. The reason why these women choose such a trend is not to attract attention or to be “on trend.” It is all about being true to themselves.

The Softening of Expressions
A smile is arguably one of the most universally appealing features a human being can possess. This feature provides instant appeal and warmth, making all conversations more approachable. However, aside from the socially beneficial aspect, there are physical effects when it comes to using one’s facial expressions consistently.
The face acts as an imprint of the most common emotional responses of a person. Constant tension or frowning can result in a face that has a permanent “hardened” look to it. Alternatively, by practicing keeping the facial expression relaxed, softening the jaw line, brows, and keeping up a friendly disposition, women actually experience aging differently.
It seems there is also an interesting “feedback loop” at play here. According to research, the simple act of smiling, whether or not it is a conscious process as opposed to an involuntary one, tends to cause the brain to produce neurotransmitters such as dopamine and serotonin. Thus, by ensuring that they maintain smiles, these ladies ensure that they continue to be happy and in good moods, thereby being more open to interaction and appearing more vibrant overall. While this may be attributed to them having fewer lines on their faces, the reason behind their lack of wrinkles is really that they smile in “happy” places.

Unsplash
Cultivating a “Lively” Mind
As we already mentioned, beauty cannot only be understood on the surface level since it has something to do with the “pilot” of our organism. Curiosity and activity of the mind create that special sparkle in the eyes and that particular zest of speech. We have all known young people who appear old since they did not learn anything new, while people over 80 can look young because they continue being interested in what is happening around them.
The scientific study of cognitive health shows that being actively engaged in thinking and learning (by reading books, learning new languages, communicating with other people, or simply solving puzzles) helps preserve brain flexibility and emotional stability. Mental activity makes our personality livelier.
A positive attitude definitely has a big part to play here too. Although getting older means you will inevitably experience things like loss and change, being able to maintain a positive outlook can help slow down your aging process. Stress has long been shown to accelerate the aging process at a cellular level. When women think about growth, exploration, and gratitude, they have a certain lightness of spirit that makes them more engaging and appealing.

Unsplash
Movement as Self-Care, Not Punishment
Exercise is always advertised as a tool to “fix” our body, yet older ladies who are energetic about aging see exercise as a necessity. Elderly women don’t train to achieve an ideal physical appearance or to compensate for eating certain foods, it simply makes them feel lively.
According to researchers, moderate physical activities are more valuable compared to sporadically performed and intense exercises. Jogging, stretching, yoga, and some exercises contribute to the improvement of blood circulation; therefore, the skin receives oxygen and nutrients that enhance its beauty. Exercise positively affects joint condition and hormone levels, which are vital to sustaining good mood and proper sleep.
Of course, exercise promotes the maintenance of muscle mass. Since our muscles tend to decrease their mass and size when aging (it is called sarcopenia), having at least some muscle mass is important to have an attractive appearance and physical capabilities. In other words, if a woman perceives exercise as self-respect, she will perform her workouts regularly and develop a healthy lifestyle. As a result, one would see that an elderly woman is active and energetic rather than exhausting herself at the gym.

Unsplash
Conclusion
Looking beautiful at any age isn’t about trying to turn back the clock. Looking beautiful at any age isn’t about trying to turn back the clock. It’s about alignment. It’s the sweet spot where how you feel on the inside, how you care for your body, and how you present yourself to the world all match.
What stands out most in women who age gracefully isn’t the absence of wrinkles or a specific dress size. It’s their presence. They seem comfortable in their own skin. They’ve built habits that support their well-being, and over time, those habits become visible in the way they stand, the way they listen, and the energy they bring into a room.
Confidence, consistency, and self-acceptance create a kind of beauty that doesn’t fade, it’s the only kind that actually improves with time. In the end, the most powerful transformation doesn’t come from a product; it comes from the quiet realization that taking care of yourself is one of the most meaningful things you can do.
Why are your veins suddenly bulging and visible?
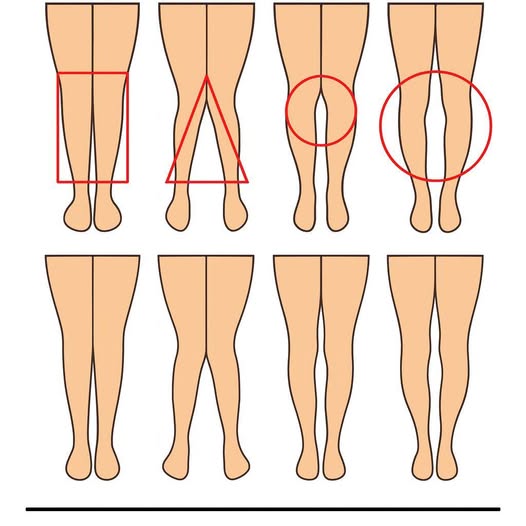
Bulging veins may actually be totally harmless when they appear on a temporary basis due to exercise or simply because it’s summer. But then again, there will be situations where the presence of bulging veins indicates the existence of a problem with your blood circulation that you should not ignore. Knowing the reason behind such an occurrence will allow you to distinguish whether it is something that requires a professional evaluation.
The vein system acts like a roadway that transports oxygen-depleted blood back up to the heart. Unlike the arterial system, which is helped by gravity, the veins have to struggle against gravity especially in the legs, using their own one-way valve system and muscle compression around them to pump blood upwards. When this system fails due to faulty valves or high pressure, blood pools up rather than moving through properly.
One of the main causes of bulging veins is simply being physically active. As you engage in physical activities, your muscles contract intensely, which in turn calls for increased blood supply, thus forcing the veins close to the skin surface. The problem is common among athletes and those with low body fat. It’s worth noting that this kind of vein visibility is not a serious health issue.

Other everyday factors include:
Ageing: With age, valves of our veins become less elastic and efficient.
Genetics: If your parents had visible veins, then there is an immense probability that you have them as well.
Hot temperatures: Hot temperature makes the blood vessels dilated (expanded).
Tight clothes: Clothes that squeeze around your waist or groin regions make pressure in your veins.
Excessive weight: Being overweight puts excessive structural strain on your legs.
Prolonged sitting or standing: Staying static defers the “muscle pump” effect, allowing blood to pool.
Although such factors might only cause temporary effects, over time, they may create conditions that lead to chronic venous problems.
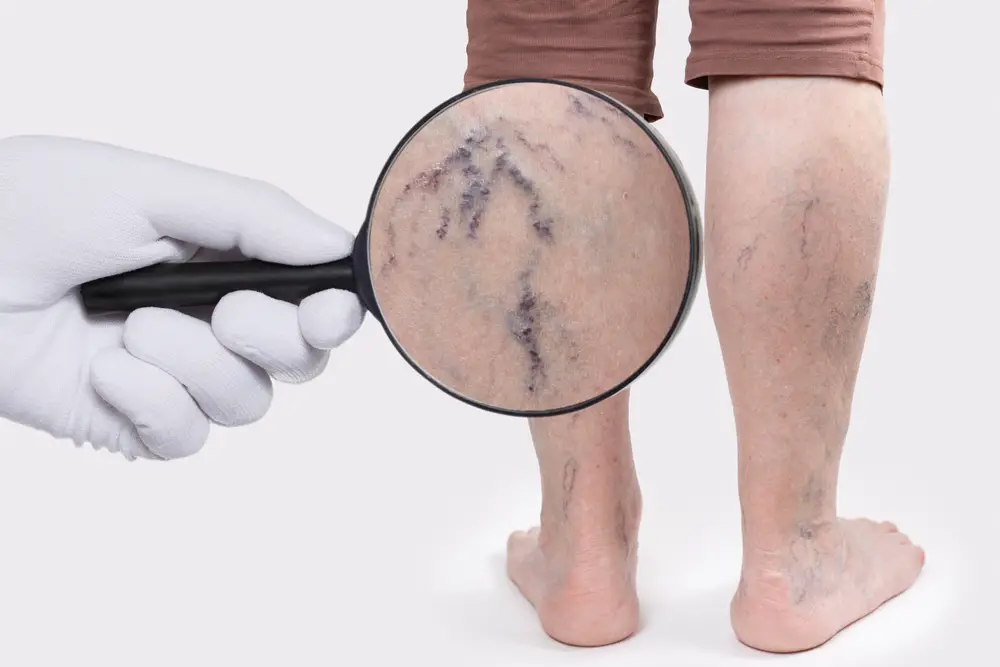
Shutterstock
In many cases, the enlarged appearance of the veins serves as an early sign of varicose veins, which belong to the spectrum of chronic venous disorders. In such a case, the inside valves become dysfunctional and cease to prevent the reverse blood flow into the vein, making it fill with blood. Varicose veins usually emerge on the legs or the feet; however, on rare occasions, they can emerge on the arms or in the pelvis area.
Usually, varicose veins have a dark blue or purple color and have a characteristic twisted appearance. While for some patients the problem does not have any symptoms apart from visual appeal, for others, the condition can be accompanied by such symptoms as a sensation of heaviness or leg ache.
According to the NHS, the underlying reason behind varicose veins is a mechanical failure. As these one-way valves fail to work effectively, the flow of blood reverses, thereby stretching the vein.

Common causes and risk factors
Some of the factors that may rapidly lead to varicose veins and bulging include:
Hormonal changes: Puberty, pregnancy, and menopause may relax vein walls.
Pregnancy: An additional strain caused by both extra blood in the body as well as an enlarged uterus putting pressure on veins in the pelvis area.
Lack of activity: Desk work or standing up for too long without walking reduces circulation.
Smoking: Smoking has been proven to damage blood vessels and affect blood circulation.
Age: The natural aging process may cause wear and tear, leading to the failure of valves.
The Mayo Clinic notes that women are statistically much more likely than men to suffer from varicose veins, especially due to hormone-related reasons.
Symptoms that shouldn’t be ignored
Whereas many cases of swollen veins may be purely superficial or temporary, certain symptoms can indicate a more serious underlying issue with blood circulation. It is advisable to consult a healthcare professional if you experience bulging veins along with any of the following symptoms:
A feeling of painful heaviness or persistent discomfort in the extremities
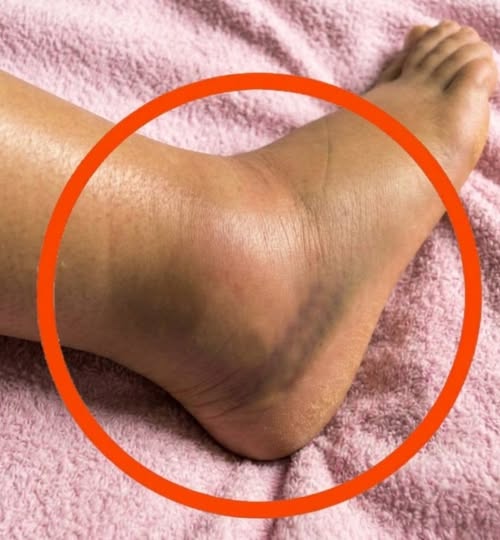
Swelling in the ankles or feet that does not improve overnight
Skin changes such as shininess, thickening, or discoloration in the affected area
Persistent itching or eczema-like irritation near the veins
Veins that feel hard, unusually warm, or tender to the touch
Sudden or rapidly worsening symptoms
One symptom that deserves particular attention is skin discoloration. This may be associated with long-term changes in circulation and reduced oxygen and nutrient delivery to surrounding tissues, which can affect skin health over time.

How varicose veins affect the body
If the valves in the vein begin to malfunction and cause the back-up of blood, the persistent pressure will deform the walls of the vein. This is because the increased pressure causes blockage to occur, preventing the skin tissues from receiving nutrients and oxygen.
If this continues without any treatment, then it may result in Chronic Venous Insufficiency (CVI), which is an incurable disease that will eventually get worse over time.
Potential complications
Untreated varicose veins can lead to serious complications.
Venous ulcers
They are open wounds characterized by pain. They occur as a result of prolonged fluid buildup which causes deterioration of the skin tissue from within. Due to poor circulation in that area, these injuries tend to be very difficult to treat and tend to recur frequently. Venous ulcers is one of the major complications of venous insufficiency, according to Cleveland Clinic.
Blood clots
The slow movement of blood provides the ideal conditions for blood clots to form. These may develop either in superficial veins called Superficial thrombophlebitis or deep inside muscles as a disease called Deep Vein Thrombosis (DVT). DVT is actually a serious condition since a fragment of the clot can detach, move towards the lungs, and lead to a pulmonary embolism. As stated by the CDC, being alert to DVTs is critical since they demand urgent medical attention.

Diagnosis and medical evaluation
Getting a diagnosis is usually straightforward. Your doctor will begin with an examination of your legs and feet from a standing position and will take your medical history into account. In order to examine what is happening inside the body, your doctor will most likely prescribe a duplex ultrasound, which is painless and non-invasive. This test will create a map of your blood flow, allowing them to determine which valves are leaking.
Treatment options
Treatment methods will be based solely on the level of severity. The milder instances of pooling may simply call for simple lifestyle modifications, while more severe instances can necessitate a fast and easy outpatient process.
Compression stockings: Elastic stockings which squeeze the leg muscles to promote upward blood flow.
Leg elevation: Putting your feet above your heart several times daily by virtue of gravity.
Lifestyle modifications: Taking walks, staying at a healthy weight, and taking breaks for physical activity.
Sclerotherapy: Injection of medicine directly into the problematic vein, thus sealing it shut safely.
Laser or Radiofrequency ablation: Sealing problem veins through use of heat energy internally.
Vein surgery: Severe instances of vein problems may require removal or bypass of the vein tract.
What it all comes down to is restoration of good circulation in the legs.

Prevention and care
While you cannot alter your genes or reverse aging, you can implement certain measures to alleviate the stress on your blood vessels:
Stay active as the body pumps blood back to your heart through movement.
Do not sit crossed-legged and do not stand in one spot for long periods of time.
Control your weight because extra weight makes the physical work more difficult for your legs.
Wear loose-fitting clothing so your waist and thighs are not constricted.
Avoid smoking since it compromises the strength of your blood vessels.
Raise your feet at the end of the day and allow your veins some relief.
The Cleveland Clinic stresses the importance of practicing a healthy routine regularly for maximum prevention of vein deterioration.
*Medical disclaimer: This article is for informational and educational purposes only and is not intended to replace professional medical advice, diagnosis, or treatment. Always seek the advice of a qualified healthcare provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay seeking it because of information you have read here.