Noticing Tiny Red Dots on Your Skin? Here’s What a Dermatologist Wants You to Know
Finding tiny red dots on your skin can be unnerving, but a dermatologist usually starts with a simple question: Did they appear slowly, or did they show up overnight? Christopher J. Haas, MD, FAAD, says many of these marks are harmless vessel growths, especially cherry angioma, which often shows up on the trunk and arms as people age. Yet timing and location can change the story fast. A gradual red speck that stays stable often points to a benign cause.
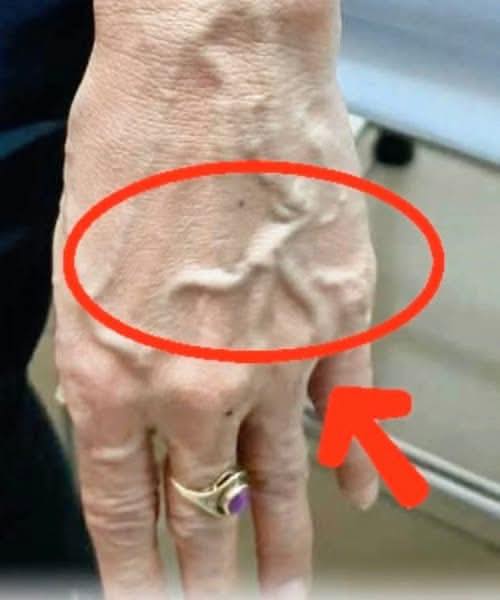
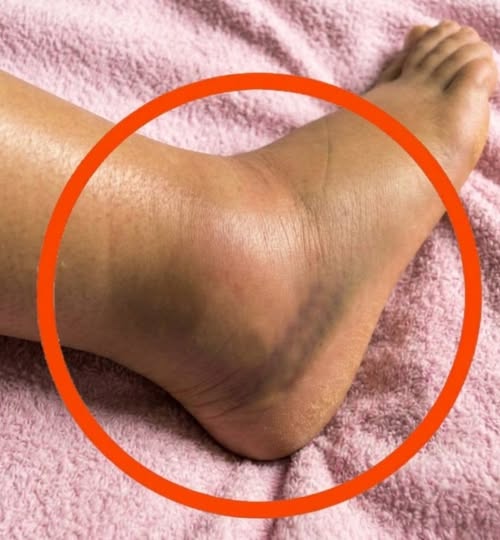
A sudden cluster that spreads over days, especially on the lower legs, can signal bleeding under the skin and needs urgent assessment. That is why dermatologists focus on clues people can track at home, like blanching with pressure, recent illness, new medications, and any unusual bruising or mouth bleeding. With those details, a dermatologist can usually sort cosmetic spots from warning signs and tell you whether to watch, book a skin check, or go straight to emergency care.
Why red dots on skin show up in the first place
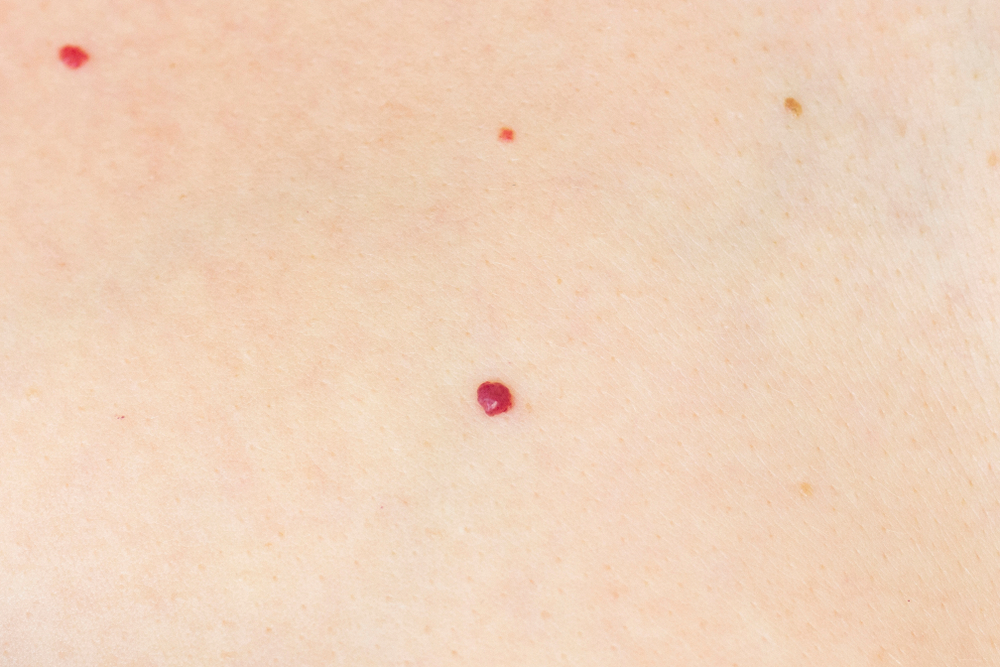
Tiny red dots on the skin often come from harmless vessel changes like cherry angioma, but sudden new spots can signal bleeding under the skin and need faster evaluation. Image Credit: Shutterstock
Many red dots on the skin look similar at first. Blood sits close to the surface in dense capillaries. When a small group of vessels widens, twists, or grows, it can create a bright pinpoint spot. Blood can also leak outside a vessel. That mechanism changes the urgency. Dermatologists start with history because the onset often solves half the puzzle. A spot that appeared over months suggests a benign vascular growth. A crop that appears over 24 to 72 hours raises different questions, especially if it spreads. They also ask what happened before the change. Furthermore, they ask about viral illness, new medicines, exercise, and skin trauma. Additionally, they ask about blood thinners, steroid creams, and supplements, because these can increase bruising or thin skin. They check whether the dots sit around hair follicles, because folliculitis can mimic a red speck.
They also ask whether the dots itch or sting, because many vascular lesions do not create symptoms unless injured. Dr. Haas points to the most common explanation in everyday practice. He notes, “What are seen most commonly, especially in patients with lighter skin tones, are cherry angiomas.” Cherry angioma is the medical name for many red moles. These spots often appear on the trunk and extremities, and they tend to multiply with age. Sun exposure can add a second category on top of that baseline. Sun damage can make superficial vessels visible. These can form fine lines or a small spider shape. A dermatologist also considers whether the “dot” is a true vascular lesion, a bruise-like bleed, or an inflamed follicle. They look for texture, scale, crust, and a persistent sore because a cancer can begin as a small pink-red spot.
If red dots on the skin arrive with fever, seek urgent care. Mouth bleeding or confusion also needs urgent evaluation. Sudden widespread spots can signal infection or a blood problem, so timing becomes critical. Even without other symptoms, a rapid change over days needs an exam. A useful home check is gentle pressure with a clear glass. Vascular spots often lighten, yet petechiae usually stay the same color. Note if the dots appear only where clothing rubs or straps press. Also note recent travel, new infections, or a new vaccine. Those clues can point toward a short-lived trigger. If the dots spread quickly, take photos and seek care the same day. Early evaluation can prevent missed serious causes. Bring a medication list, including supplements, to appointments.
Cherry angioma, the common “red mole” that usually stays harmless
Cherry angioma tends to earn its reputation as the classic harmless red dot on the skin. It is a benign overgrowth of small blood vessels. Many start as tiny flat red marks, then become a small dome that can bleed if scraped. People often notice them after showers or while applying lotion because water and friction make the color stand out. They show up most often on the torso, upper arms, and thighs. They can appear anywhere, but palms and soles are less typical. Genetics, age, and pregnancy can influence how many form. Clinicians still cannot name one cause for each spot. Many people develop their first lesions after 30, then notice a slow increase over the years. That gradual pace is one reason dermatologists often reassure patients once the exam fits the classic look. Cleveland Clinic estimates that about 50% of adults have cherry angiomas after age 30.
It also reports they are common by age 75. Those numbers fit normal aging. Large health systems describe them in plain language because they are so common. Cleveland Clinic states,“Cherry angiomas are small, red bumps on your skin that are harmless to your overall health.” Cleveland Clinic also notes that they commonly appear after age 30. Sun exposure does not cause every cherry angioma. Yet sun-damaged skin can make them look more obvious. Cherry angiomas also tend to look uniform in color, round, and sharply defined. If a red dot looks irregular, scaly, tender, or rapidly enlarging, a dermatologist may consider a different diagnosis. Those include pyogenic granuloma, which can bleed easily, or an early skin cancer that presents as a pink-red bump.
A dermatologist may use dermoscopy to inspect vessel patterns. If uncertainty remains, a small biopsy can settle the diagnosis quickly and rule out uncommon mimics. When removal is cosmetic, dermatologists still discuss trade-offs. Cleveland Clinic notes removal can cause scarring and warns people not to remove angiomas at home. At-home cutting or tying off can lead to infection and uncontrolled bleeding. In the clinic, a doctor can numb the skin, remove the lesion, and give wound care instructions that lower complication risk. If a cherry angioma bleeds after a bump, treat it like a wound. Clean it, apply antibacterial ointment, and cover it.
Bleeding often looks dramatic because the lesion contains vessels, but it usually stops with firm pressure. If bleeding keeps restarting, medical care can seal the vessel and prevent infection. If you notice one that starts bleeding often, mention it at your next skin check. Frequent bleeding can happen in high-friction areas, like waistbands or bra lines. Some people also bleed more easily when they take blood thinners. A dermatologist can confirm it is a cherry angioma and then remove it safely. Many removals take only minutes in the office. The doctor may also send tissue to a lab if the spot looks atypical. That step can rule out rare mimics. Between visits, take a clear photo to track size and color.
Telangiectasia and sun damage, when “red dots” are really visible surface vessels
Some red dots on the skin are not dots at all when viewed up close. They are widened vessels near the surface. They can look like thin lines or a tiny red star. The umbrella term is telangiectasia. People often notice them on the nose, cheeks, and upper chest. These areas take years of sun. Heat and alcohol can worsen them. Topical steroid overuse and rosacea also contribute. Sun exposure is a frequent background factor. These vessels can also become more visible as skin thins with age. People sometimes confuse telangiectasia with petechiae because both can appear as small red marks. Their behavior under pressure differs. Telangiectasia often forms a branching shape. Petechiae tend to remain as dots. A quick look with magnification can reveal the difference. Many people only examine the area closely once worry sets in.
DermNet NZ explains, “Telangiectasia is a condition in which there are visible small linear red blood vessels (broken capillaries).” The word “broken” can mislead people. In most cases, the vessel wall has not ruptured. The vessel has dilated and become easier to see, especially in thin facial skin. Dermatologists often use a blanching test to separate a superficial vessel from bleeding under the skin. Merck Manual describes diascopy: “A microscope slide is pressed against a lesion (diascopy) to see whether it blanches.” Vascular marks often lighten. Petechiae usually do not. Treatment depends on goals. Many people leave telangiectasia alone. If removal is desired, dermatologists use vascular lasers or intense pulsed light. They adjust settings for skin tone to reduce pigment changes. Prevention relies on daily sunscreen and hats, because ultraviolet damage can create new visible vessels even after treatment.
If facial flushing accompanies the vessels, a dermatologist may also screen for rosacea and discuss trigger control. They may adjust skin-care routines because harsh scrubs can increase redness. These steps can reduce how noticeable the marks become over time. When people choose laser or light therapy, the dermatologist often plans several sessions. They also advise strict sun protection after treatment. Tanning can increase pigment complications. The goal stays practical: reduce redness without trading it for blotchy discoloration. Daily sun protection also helps limit new visible vessels over time, especially on the nose, cheeks, and upper chest. Choose a broad-spectrum SPF 30 or higher, and apply enough to fully cover the area.
If you sit near windows or drive often, remember that UVA can still reach the skin. Gentle cleansing matters too. Hot water, rough scrubs, and alcohol-heavy toners can keep facial redness active, which makes telangiectasias stand out. If you use retinoids or acne treatments, introduce them slowly, because irritation can add extra redness in the short term. For persistent flushing, a dermatologist may discuss prescription options that reduce redness and vessel dilation. If you want cosmetic improvement, ask what device fits your skin tone and vessel type, because lasers and intense pulsed light use different targets. After treatment, strict sun avoidance lowers the risk of post-treatment dark marks.
Petechiae, purpura, and low platelets, when red dots on skin can signal urgency
Petechiae look like tiny red or purple pinpoints that appear suddenly. They often cluster on the lower legs and ankles. Gravity increases pressure during standing and walking. Unlike a cherry angioma, petechiae do not rise above the skin surface. They also do not blanch with pressure because blood has leaked into the skin. MedlinePlus states, “Areas of bleeding into the skin do not become paler (blanch) when you press on the area.” That clue helps. Timing and symptoms still matter. Clinicians use size terms that can help you describe what you see. StatPearls notes that petechiae measure less than 2 mm, while larger non-blanching spots are purpura. Petechiae can follow a clear trigger such as forceful coughing, vomiting, heavy lifting, or a long workout. In those cases, the dots often fade within days, and the person otherwise remains well.
Petechiae can also appear where clothing or straps create repeated pressure. A clinician still checks for bruises, gum bleeding, or heavy menstrual bleeding. Those signs can travel with low platelets. Petechiae can also reflect a platelet problem, and that possibility drives urgency. Platelets help blood clot, so a low platelet count can lead to pinpoint bleeding. NHLBI lists petechiae as a sign of immune thrombocytopenia. It defines them as “small, flat red spots under the skin caused by blood leaking from blood vessels.” Low platelets can follow illness or medicines. Immune disease can also play a role. They can also arise from bone marrow disease.
Clinicians avoid casual reassurance when the dots appear quickly, spread, or come with bruising that has no clear injury. Cleveland Clinic states: “If you have pinpoint-sized red dots under your skin that spread quickly, or petechiae plus other symptoms, seek medical attention.” Clinicians often order a complete blood count on the same day. They also review recent infections and medicines. Quick testing can show if the issue stays in the skin. It can also reveal a blood problem needing treatment. Even when tests are normal, the visit can rule out dangerous infections. It also gives a documented baseline for follow-up rash. If the dots appear on the whites of the eyes or inside the mouth, mention it immediately. Those sites can signal a wider bleeding tendency.
Clinicians also check for a rapidly spreading rash with fever, because some infections become dangerous fast. The CDC notes that meningococcal disease can include a petechial or purpuric rash, alongside sudden fever and other symptoms. If you cannot link the spots to a clear trigger, do not wait weeks to watch them. Mayo Clinic advises, “See a member of your health care team soon if you develop petechiae all over the body, or you can’t identify the cause of the petechiae.” Even when blood counts return to normal, the visit can still help. A clinician can confirm blanching, check vitals, and decide if you need follow-up testing. If you take blood thinners, ask whether dosing or interactions could contribute. If a child develops a non-blanching rash, treat it as a same-day assessment, unless a clear mechanical cause exists. Keep the photo timeline, because speed guides decisions.
What a dermatologist checks, and when a “red dot” needs a skin cancer workup

Dermatologists assess timing, location, blanching, and lesion features to rule out serious causes, including skin cancer, and a biopsy remains the only definitive way to confirm cancer when a spot looks suspicious. Image Credit: Shutterstock
Dermatologists do not treat every red dot on the skin as cancer. They do treat uncertainty as a reason to examine. They look at the lesion and the surrounding sun damage. Chronic ultraviolet exposure raises cancer risk. People often expect melanoma to look dark. Yet it can show up as a new, unusual spot. Melanoma can appear in more than one way, including as an unusual new spot. That advice can still apply to pink or red lesions. A new lesion on the scalp or ears deserves attention. The face, chest, and forearms do too. These areas accumulate sun over decades. Dermatologists also note spots on scars and chronic sores. Repeated crusting after “healing” can also be a warning. These stories can fit basal cell or squamous cell cancer. A dermatologist’s exam blends pattern recognition with bedside tests and tools.
They check whether the spot blanches, whether it has scale or crust, and whether it bleeds with minimal contact. They ask how long it has been present and whether it has changed in size, shape, color, or symptoms. Dermoscopy helps identify vessel structures that suggest a benign angioma or a suspicious tumor. Dermatologists also use the rest of your history. They ask about sunburns, tanning beds, and outdoor work. They ask about a family history of melanoma. Furthermore, they ask about immune suppression after transplant or chemotherapy. They also ask about new medicines that affect bleeding. This includes aspirin and anticoagulants. They sometimes examine nails and the inside of the mouth. For people with many red dots on their skin, the visit can include education. The dermatologist explains what is normal for you.
They explain which spots deserve photos, and which deserve a visit. If your spots sit in a friction zone, they may suggest covering them. That can stop repeated bleeding. They can also offer a simple plan for follow-up. A set recheck can be useful after a biopsy. It also helps after a new rash that was not fully explained. At home, check the same areas each month. Use a mirror for the back and scalp. Keep notes on any spot that changes or bleeds. Sunscreen does not erase existing angiomas, but it can limit new sun damage. Choose broad-spectrum protection and reapply during long outdoor days. These steps reduce future surprises during routine skin checks. Protective habits can also slow new telangiectasia on the face and upper chest over the next few years.
If you take your own photos, bring them, because they can show the pace of change. That timeline can influence whether the dermatologist watches, treats, or biopsies. If the spot looks worrisome, a biopsy provides the answer. AAD explains, “Having a skin biopsy is essential. It’s the only way to know whether you have skin cancer.” When the diagnosis is benign, treatment stays optional. Dermatologists can remove a cherry angioma for bleeding or irritation. They can also remove it for cosmetic concerns. They may use cautery or laser in the office. For petechiae, the dermatologist usually coordinates urgent medical evaluation because the cause often sits outside the skin. For cancers, early detection often leads to simpler treatment overall. A prompt exam can turn anxiety into a clear plan quickly.
6 habits that make older women look beautiful
The idea of beauty is one of those rare things in life that becomes more intriguing as time goes by. When we are young, beauty is a purely biological thing, something that happens because of our genetic makeup and our youthful, smooth skin. But as we age, so does our understanding of beauty. Not only does beauty not disappear; it changes, becoming more complex and profound. It evolves from an aesthetic aspect into a deeper notion.
Many women become elegant in a certain way. They develop an aura of quiet confidence, poise, and charisma that is unique to them and impossible to buy or copy. Their beauty doesn’t come as a result of trendy, costly procedures and treatments, but is the product of habits cultivated over many years.
Instead of seeking perfection, which is an impossible and ultimately tiresome goal by its very definition, it’s more realistic to focus on growth and self-respect.
The following is an analysis of several traits that make up a woman’s natural beauty as she matures, as well as the rationale behind why they work for her mind and body.

The Art of Posture and Intentional Movement
A person’s posture can say more before any hello than their actual words. Body language is perhaps the most primitive means of communication and conveys what the mind truly feels. Standing straight, keeping one’s shoulders relaxed instead of hunched up by the ears, and moving with purpose convey an impression of self-confidence.
Of course, as people age, some deterioration of posture occurs. This can be attributed to the weakening of muscles, decreased bone density, and the effects of years of poor posture, which often develop from sitting too long at a desk or staring at smartphones. However, recent discoveries in the science of “embodied cognition” have shown that posture does not only affect other people’s perception but also influences one’s inner state. When a person stands tall, they do not only “pretend” to be confident—they signal to their brain that they are comfortable and in control of their surroundings.
Women who pay attention to maintaining good posture look more lively and youthful, since they do not seem to “age down” into themselves. A smooth, stable walking pattern, together with an upright posture, helps create a sense of elegance that has nothing to do with what brand name one wears or how professionally one’s make-up is applied.

Radical Consistency in Self-Care
Good skin is not about an elaborate and lengthy nighttime regimen of cutting-edge ingredients. Instead, dermatological studies continually emphasize one simple yet critical truth: consistency wins over complexity. Women who radiate health despite their advanced age are often those who have stopped playing around with each new trend and developed a trustworthy and basic routine.
Skincare for graceful aging can be simplified to the three core steps: cleansing, moisturizing, and protection. In particular, the latter step is proven to be crucial to prevent premature aging of the skin. It is believed that 80% to 90% of visible signs of skin aging, such as wrinkles, dryness, and uneven skin tone, are due to excessive exposure to the sun. For instance, women who apply a daily layer of SPF for twenty years differ noticeably from those who only do so when going to the beach.
The next pillar is moisturization. As you get older, your skin barrier weakens, becoming less effective at retaining lipids and moisture. By hydrating the skin, you support this barrier, which keeps the skin soft, glowing, and more resistant to damage from external factors. It’s not about how expensive the jar is, it’s about consistency. These women care for their skin as an investment, not as an emergency that requires miracle fixes.
Personal Style Over Fleeting Trends
There is a vast difference between being “fashionable” and “having style.” The former dictates what one should wear according to fashion industry standards each month, while the latter is choosing to wear clothes that define one’s identity. In the development of one’s sense of beauty, many ladies experience a significant boost in confidence once they cease trying to fit in with fashion standards tailored to adolescents and begin building an individual aesthetic reflective of who they are now.
It is important to note that this is not about one’s selfish interests but rather a phenomenon known as “enclothed cognition.” The hypothesis posits that the clothing one wears can actually affect their psychology. When women dress themselves up in clothes that suit their body type, make them feel comfortable, and reflect their character.
As women age and become unique in their looks, they usually go for clothing that complements their body and accentuates their facial features rather than concealing their true beauty by wearing clothes that are too big for them or too small. Women who have unique looks usually become experts at color matching. They know what colors bring out the best in them and which colors are just not flattering. The reason why these women choose such a trend is not to attract attention or to be “on trend.” It is all about being true to themselves.

The Softening of Expressions
A smile is arguably one of the most universally appealing features a human being can possess. This feature provides instant appeal and warmth, making all conversations more approachable. However, aside from the socially beneficial aspect, there are physical effects when it comes to using one’s facial expressions consistently.
The face acts as an imprint of the most common emotional responses of a person. Constant tension or frowning can result in a face that has a permanent “hardened” look to it. Alternatively, by practicing keeping the facial expression relaxed, softening the jaw line, brows, and keeping up a friendly disposition, women actually experience aging differently.
It seems there is also an interesting “feedback loop” at play here. According to research, the simple act of smiling, whether or not it is a conscious process as opposed to an involuntary one, tends to cause the brain to produce neurotransmitters such as dopamine and serotonin. Thus, by ensuring that they maintain smiles, these ladies ensure that they continue to be happy and in good moods, thereby being more open to interaction and appearing more vibrant overall. While this may be attributed to them having fewer lines on their faces, the reason behind their lack of wrinkles is really that they smile in “happy” places.

Unsplash
Cultivating a “Lively” Mind
As we already mentioned, beauty cannot only be understood on the surface level since it has something to do with the “pilot” of our organism. Curiosity and activity of the mind create that special sparkle in the eyes and that particular zest of speech. We have all known young people who appear old since they did not learn anything new, while people over 80 can look young because they continue being interested in what is happening around them.
The scientific study of cognitive health shows that being actively engaged in thinking and learning (by reading books, learning new languages, communicating with other people, or simply solving puzzles) helps preserve brain flexibility and emotional stability. Mental activity makes our personality livelier.
A positive attitude definitely has a big part to play here too. Although getting older means you will inevitably experience things like loss and change, being able to maintain a positive outlook can help slow down your aging process. Stress has long been shown to accelerate the aging process at a cellular level. When women think about growth, exploration, and gratitude, they have a certain lightness of spirit that makes them more engaging and appealing.

Unsplash
Movement as Self-Care, Not Punishment
Exercise is always advertised as a tool to “fix” our body, yet older ladies who are energetic about aging see exercise as a necessity. Elderly women don’t train to achieve an ideal physical appearance or to compensate for eating certain foods, it simply makes them feel lively.
According to researchers, moderate physical activities are more valuable compared to sporadically performed and intense exercises. Jogging, stretching, yoga, and some exercises contribute to the improvement of blood circulation; therefore, the skin receives oxygen and nutrients that enhance its beauty. Exercise positively affects joint condition and hormone levels, which are vital to sustaining good mood and proper sleep.
Of course, exercise promotes the maintenance of muscle mass. Since our muscles tend to decrease their mass and size when aging (it is called sarcopenia), having at least some muscle mass is important to have an attractive appearance and physical capabilities. In other words, if a woman perceives exercise as self-respect, she will perform her workouts regularly and develop a healthy lifestyle. As a result, one would see that an elderly woman is active and energetic rather than exhausting herself at the gym.

Unsplash
Conclusion
Looking beautiful at any age isn’t about trying to turn back the clock. Looking beautiful at any age isn’t about trying to turn back the clock. It’s about alignment. It’s the sweet spot where how you feel on the inside, how you care for your body, and how you present yourself to the world all match.
What stands out most in women who age gracefully isn’t the absence of wrinkles or a specific dress size. It’s their presence. They seem comfortable in their own skin. They’ve built habits that support their well-being, and over time, those habits become visible in the way they stand, the way they listen, and the energy they bring into a room.
Confidence, consistency, and self-acceptance create a kind of beauty that doesn’t fade, it’s the only kind that actually improves with time. In the end, the most powerful transformation doesn’t come from a product; it comes from the quiet realization that taking care of yourself is one of the most meaningful things you can do.